I was diagnosed with Type 1 diabetes (T1D) in 2008 at 10 years of age.
Now as a nearly 25-year-old woman, I have seen the many ups and downs diabetes management can take.
My diabetes has greatly impacted my mental health, and at my lowest point of diabetes management it has even resulted in hospitalization.
I have been utilizing a continuous glucose monitoring device (CGM) since 2018. Photo credit: Alexa Gregoris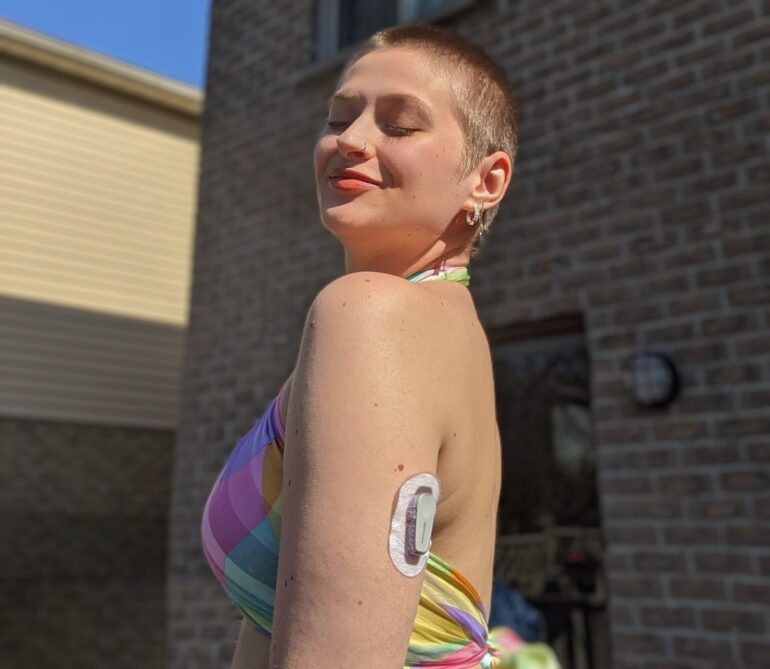
Type 1 diabetes is affected by 42 factors at any given moment, and diabetics make around 180 health-related decisions a day to stay alive – on top of responsibilities of everyday life.
Devices like continuous glucose monitoring (CGM) sensors have revolutionized diabetes management, and greatly improve self-management and diabetic burnout prevention.
CGM devices are small wearable sensors that monitor blood sugar levels continuously and notify users of high or low blood sugar levels so diabetics can adjust insulin intake and be aware of risks.
The Juvenile Diabetes Research Foundation (JDRF) said CGM devices lead to better glycemic control and lessens the risk of Type 1 diabetic complications.
In recent years the number of people who are not diabetic using CGM devices has increased.
CGM devices are being marketed as weight loss gadgets and a form of trendy precision nutrition.
Forbes published an article claiming glucose monitoring is a next-generation tool for weight loss management.
“Biohack your way to weight loss,” Rebecca Suhrawardi from Forbes wrote.
“Aside from weight loss, being able to monitor foods in this detailed way is what makes CGM as trendy as it is—it’s another tool in the growing desire for personalized nutrition,” she said.
CGM technology is a life changing device for those living with diabetes.
To market CGM devices simply as a weight loss gadget is not only irresponsible, but deeply ableist.
These devices are being taken out of the hands of those who require them to live comfortably.
“Continuous glucose monitoring devices help improve self-management of T1D by regulating overall blood sugar, enabling people to spend more time in target range and relieving them of the anxiety that surrounds the disease, as well as aiding them to achieve excellence in exercise and in life,” JDRF said.
Dexcom Canada said their CGM devices are recommended only for those living with Type 1 or Type 2 diabetes, or those experiencing hypoglycemia. Photo credit: Dexcom Canada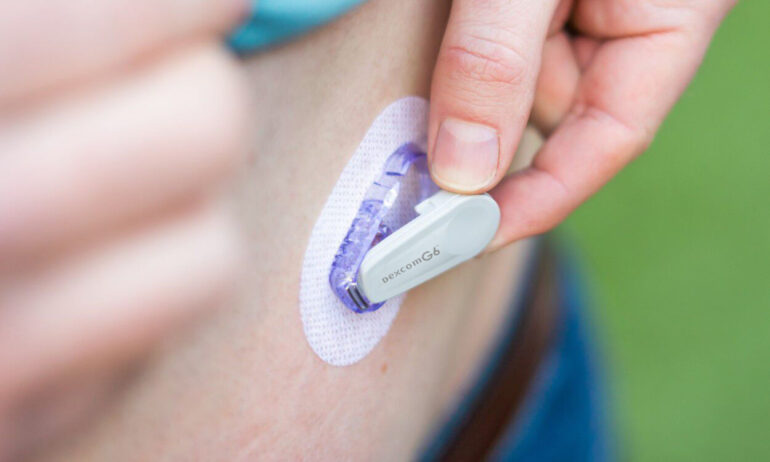
Non-diabetics will not receive accurate health data from CGM devices, as their metrics were invented specifically with diabetic bodies in mind.
Dr. Viral N. Shah, associate professor at the Barbara Davis Center for Diabetes in Colorado, said it is possible CGM devices may even misclassify non-diabetics as prediabetes.
“If people without diabetes use CGM, they have to remember that most CGM metrics, such as time in range or time below range or GMI (glucose management indicator), were developed for people with diabetes and not for people without diabetes,” he said.
“People without diabetes should not be using these metrics to assess their health status or changes in health status,” Shah said.
For diabetics CGM devices are not easily accessible.
Even without non-diabetics purchasing CGM devices for unnecessary use, only a limited number of diabetics have access to such devices.
CGM technology is not covered under provincial health insurance plans.
“Canadians with T1D whose private or group insurance plan does not include CGM or who have no such insurance must go out-of-pocket,” JDRF said.
Those who can afford to access CGM devices are spending hundreds of dollars every month, on top of the price of insulin and other diabetic technology and healthcare services.
I spend $100 per Dexcom G6 CGM sensor, which only lasts 10 days before it needs to be changed.
Type 1 diabetes feels like a full-time job all on its own, without any paycheck.
To live with a chronic disease that is stigmatized and often invisible to the public eye is overwhelming enough, without having to fight able-bodied individuals to access life changing technologies that were made for us.

